Women and Maternal Mental Health & Psychiatry
Women and Maternal Mental Health & Psychiatry

For a variety of Medical and Biological reasons there are differences in health and illness between male and female genders. Some mental and physical diseases are more prevalent among men and some more prevalent among women. Females as a gender face specific Mental Health challenges unique to their gender. In our modern time women, as a gender, are assuming more social, economic, relational, family and occupational responsibilities. These responsibilities, along with unique nature of health and illness for women, can result in significant emotional and mental distress for women that if left unattended will cause numerous health concerns at major cost. When a woman falls sick, everybody around her suffers!
Unfortunately, due to these factors and a host of other reasons, women as a gender, in the past and even at the present, have been marginalized and subjected to social and economic restriction worldwide.
Mental Health challenges for women are more prominent in certain periods in their life cycle including; Menarche (when women start menstruating), Menstruation periods, Pregnancy, Delivery and Menopausal phases. These challenges are partly medical and relating to chemical and hormonal changes in the brain and body and partly relating to psychological stresses that these changes create. Among these phases, Pregnancy and Delivery pose special and unique mental and emotional conditions. Majority of female susually get through these challenges uneventfully. In certain situations however, the Mental and Emotional changes are so severe and out of proportion that demands Medical and Professional Care.
The Co-occurring Mental Illness such as; Addiction, Depression, Bipolar and Anxiety disorders, along with Ante-Natal Depression (AND) or Post-Partum Depression (PPD), are far more complex and vicious and affect the new moms and their babies more seriously.
For these reasons, American College of Obstetrics and Gynecology recommends that OB-GYNs screen their patients for depression and other Maternal Mental Health Issues and help them get treatment for depression and other Maternal Mental Health Issues and help them get treatment
Specific Gender related Mental Health concerns for women are numerous and include:
- Menarche (when women start menstruating):
Menarche, is a Greek term, it is the first menstruation, or first menstrual bleeding, in female humans. From both social and medical perspectives, it is often considered the central event of female puberty, as it signals the possibility of puberty and fertility.
Menarche is the first menstrual period in adolescent girls and occurs at an average age of 13.5 years. It is however reported that some girls had menarche as early as 9 years old. Menarche marks the beginning of the reproductive phase in the life of a woman. Menarche is memorable and significant event for girls. The onset of menarche is largely influenced by genetic factors. However, body fat composition, eating behavior, physical training, and psychosocial stress can also impact on the timing of menarche. For example, obesity and stressful life events prior to menarche including parental divorce, absence of a father, maternal mood disorders, presence of a stepfather, or an unrelated man at home are factors associated with earlier menarche. In contrast, excessive dieting, physical training, and thinness are related to a delayed onset.
Girls reaching menarche earlier than their peers tend to worry more about menstruation, experience menstruation less positively, experience depression, become more likely victims of peer sexual harassment, and are more likely involved in deviant behavior. Menarche may have a positive personal significance insofar as it is associated with greater maturity, but this positive impact is overshadowed by a negative interpersonal significance as girls become increasingly self-conscious, embarrassed, and secretive.
Factors influencing the psychological impact of menarche include age at time of 1st period, social factors, amount of preparation, and cultural factors.
The degree to which young girls are prepared for menstruation varies. Often they receive information from their mothers, female peers, and the media.
Earlier ages at menarche are associated with higher rates of both depressive symptoms and antisocial behaviors in early-middle adulthood if difficulties that started in adolescence were not treated.
Menarche is the culmination of a series of physiological, anatomic, psychological and mental changes of the puberty. These developments include:
- Attainment of a sufficient body mass (typically 17% body fat).
- Secretion of Sex Hormones including estrogen by the ovaries
- Over an interval of about 2 to 3 years, estrogen stimulates growth of the uterus, height, breast, widening of the pelvis, and increased fat tissue in certain hips and belly.
- Estrogen stimulates growth and vascularity of the endometrium, (the inner lining of the womb).
- Death of some of the endometrial tissue (the inside lining of the womb) from these hormone or blood supply fluctuations leads to sloughing of part of the lining with some blood flow from the vagina (menstruation).
- Psychological changes: The time around Menarche is a time of inner turmoil for young women. It is the time for spurts of intense but poorly defined sensations. This turmoil is related to the increased flow of hormones with bodily changes which warns the onset of menarche. There are some psychological confusion that is induced by these body changes which are compounded by social and cultural factors and pressure. In some cultures, there are unhygienic and negative connotations associated with menstruation. This factors compound the physical changes and mental confusions associated with menarche. In his phase confusion about body image and sexual identification is not uncommon. In all cultures, Menstruation defines the sexual role and identity. This combination of physical changes along with mental confusions and conflicts is usually associated with complex and unexplainable symptoms such as headache, nausea vomiting and irritability.
These young women at this phase are the prime candidate for unnecessary medical and diagnostic procedure. It is during this time that young women are specifically vulnerable to some psychological and mental distress.
As much a significant number of young women transition from the turbulent years of adolescent and menarche related mental distress, for a lot of reason, some adolescents do not recover well. The mental distress of this phase leads to a variety of psychiatric and behavioral disorders including:
- Obesity
- Anorexia
- Bulimia
- Sexual acting out
- Incidental pregnancy
- Tobacco Alchohol and Drug Abuse
- Depression
- Mood Swings
- Anxiety
- Truancy
- Driving Accidents
- Antisocial behavior, (Petty theft, lack of respect for the right of others, shoplifting)
Studies have demonstrated that early menarche and untreated mental and behavioral disorder during this period has serious and lasting effects on young women that will last beyond their adolescence and way into their adulthood.
- Menstruation and Mental Health:
Hormonal changes and psychological changes before and during and even after each mensural period are mostly tolerable for a great number of women. In certain cases however these changes are so severe that may result in mental health distress and affect other aspects of a woman’s life. These conditions used to be referred to as “premenstrual stress disorder’ and was usually regarded insignificant in the past. Growing research evidence however indicated that left untreated, the mental health changes and distress women endure not only causes suffering and pain, it is also costly in terms of other associated relational and medical problems and down time at home and work. These conditions gained recognitions and its rightful position in last edition of the Diagnostic Manual of Mental Disorders as follows.
Premenstrual Dysphoric Disorder (PMDD) is a health problem that is similar to premenstrual syndrome (PMS) but is more serious. PMS causes:
- Severe irritability
- Depression or Anxiety in the week or two before your period starts. Symptoms usually go away two to three days after your period starts. You may need medicine or other treatment to help with your symptoms.
PMDD is a condition similar to PMS that also happens in the week or two before your period starts as hormone levels begin to fall after ovulation. PMDD causes more severe symptoms than PMS, including severe depression, irritability, and tension.
Who gets PMDD?
PMDD affects up to 5% of women of childbearing age. Many women with PMDD may also have anxiety or depression.
Symptoms of PMDD include:
- Lasting irritability or anger that may affect other people
- Feelings of sadness or despair, or even thoughts of suicide
- Feelings of tension or anxiety
- Panic attacks
- Mood swings or crying often
- Lack of interest in daily activities and relationships
- Trouble thinking or focusing
- Tiredness or low energy
- Food cravings or binge eating
- Trouble sleeping
- Feeling out of control
- Physical symptoms, such as cramps, bloating, breast tenderness, headaches, and joint or muscle pain
What causes PMDD? Researchers do not know for sure what causes PMDD or PMS. Hormonal changes throughout the menstrual cycle may play a role. A brain chemical called serotonin may also play a role in PMDD. Serotonin levels change throughout the menstrual cycle. Some women may be more sensitive to these changes. How is PMDD diagnosed? Your doctor will talk to you about your health history and do a physical examination. You will need to keep a calendar or diary of your symptoms to help your doctor diagnose PMDD. You must have five or more PMDD symptoms, including one mood-related symptom, to be diagnosed with PMDD. Treatments for PMDD:
- Treatment of PMDD is usually a combination of Health Counseling also known as talk therapy and medications. The proportions of these measures depend on each woman special conditions.
- Stress management, such as relaxation techniques and spending time on activities you enjoy.
Making healthy changes, such as eating a healthy combination of foods across the food groups, cutting back on salty and sugary foods, and getting more physical activity, may also help relieve some PMDD symptoms. But PMDD can be serious enough that some women should go to a doctor or nurse to discuss treatment options. And, if you are thinking of hurting yourself or others, call 911 right away.
- Pregnancy and Mental Health:
Specific Gender related mental Health concerns relating to woman include what is referred to as Ante-Natal-Depression (AND), (Ante, meaning BEFORE, Natal meaning BIRTH) and Post-Partum-Depression (PPD), (post meaning AFTER, Partum meaning BIRTH). Mental Health problems following child birth, also known as Postpartum Mental Disorders also includes Postpartum Obsessive Compulsive Disorders and Anxiety Disorders and Postpartum Traumatic Stress Disorder.
Data suggest that 49.9% of women with Depression “Before”, (AND) and 30.8% of women with Depression “After” (PPD), delivery, are identified in clinical settings; ONLY 13.6% of women with (AND) and 15.8% of women with PPD receive treatment.
In fact, ONLY 8.6% of women with (AND) 6.3% of women with PPD receive professional treatment; and ONLY 4.8% of women with (AND) and 3.2% of women with PPD achieve complete recovery.
An estimated 1 in 7 pregnant women and new mothers become clinically depressed during pregnancy or postpartum. But their primary point of contact in the medical system is their obstetricians who often are not trained and lack the skills to address Psychiatric Problems. As a result, few women get a diagnosis or treatment. According to one study, less than 20% of women get treated. Untreated maternal mental health issues leads to un-necessary suffering of new moms and results in very high cost. For example, untreated perinatal anxiety and mood disorders cost the state of California $2.4 billion for all births in 2017, when mother-infant pairs were followed for 5 years.
Untreated perinatal depression affects not just the mother's health, but also her baby's and her entire family's social and emotional well-being. It can increase the risk of premature birth and low birth weight babies. And when a new mom is depressed, it affects her ability to take care of her baby and bond with it. That in turn can affect the baby's physical and emotional development and even puts it at a higher risk of having mental health problems later in life. Serious depression in parents and caregivers can affect the children in their care. When children grow up in an environment of mental illness, the development of their brains may be seriously weakened, with implications for their ability to learn as well as for their own later physical and mental health.
Following childbirth, also known as "postpartum", women may experience postpartum disorders that can affect their mental health. The high hormonal changes and fluctuations that occur during and after childbirth could cause mothers to feel intense mood swings called "the baby blues" which affects 80% of mothers. If symptoms persist for more than a couple weeks, or interfere with marriage, normal responsibilities at home and work, then it could potentially be something more severe such as a postpartum disorder and requires psychiatric care.
How frequent is Postpartum Disorders:
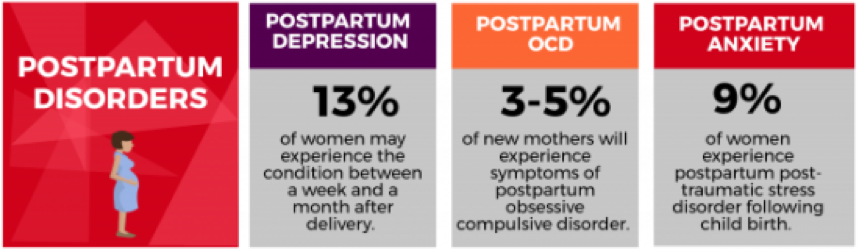
Types of Postpartum Disorders:
- Postpartum Depression, or PPD, is a mood disorder in women shortly after childbirth. Mothers with PPD experience feelings of extreme sadness, anxiety, and exhaustion that can affect the woman's ability to care for herself or for others. Signs and symptoms for PPD are the same as those for clinical depression. In women with postpartum depression, symptoms usually begin within the first four weeks of giving birth, although some women report decreasing mood in the late third trimester of pregnancy.
Signs and Symptoms of Postpartum Depression
- Feelings of emptiness and hopelessness
- Irritability, anxiousness, and guilt
- Feelings of exhaustion, severe tiredness
- Feelings of tension
- Loss of interest and energy
- Inability to concentrate or remember details
- Suicidal thoughts or attempts of suicide
- Changes in appetite – eating too much or too little
- Physical symptoms – aches and pains, cramps, headaches, digestive issues, breast tenderness, bloating
- Mood swings
- Panic Attacks
- Sleep disturbances; sleeping too much or too little, insomnia
- Postpartum Obsessive-Compulsive Disorder (OCD) is one of the most misunderstood perinatal disorders. Women with OCD often tend to attribute the onset or worsening of their symptoms to pregnancy or delivery. Postpartum Obsessive-Compulsive Disorder (OCD) is the most misunderstood and misdiagnosed of the perinatal disorders. You do not have to be diagnosed with OCD to experience these common symptoms of perinatal anxiety. It is estimated that as many as 3-5% of new mothers and some new fathers will experience these symptoms. The repetitive, intrusive images and thoughts are very frightening and can feel like they come “out of the blue.” Research has shown that these images are anxious in nature, not delusional, and have very low risk of being acted upon. It is far more likely that the parent with this symptom takes steps to avoid triggers and avoid what they fear is potential harm to the baby.
Symptoms of perinatal Obsessive-Compulsive symptoms can include:
- Obsessions, also called intrusive thoughts, which are persistent, repetitive thoughts or mental images related to the baby. These thoughts are very upsetting and not something the woman has ever experienced before.
- Compulsions, where the mom may do certain things over and over again to reduce her fears and obsessions. This may include things like needing to clean constantly, check things many times, count or reorder things.
- A sense of horror about the obsessions
- Fear of being left alone with the infant
- Hypervigilance in protecting the infant
- Moms with postpartum OCD know that their thoughts are bizarre and are very unlikely to ever act on them.
Risk Factors
Risk factors for postpartum OCD include a personal or family history of anxiety or OCD.
Postpartum OCD is temporary and treatable with professional help. If you feel you may be suffering from one of this illness, know that it is not your fault and you are not to blame. You can use our resource page to reach out now. We understand what you are going through and will connect you to people who understand and can help.
Postpartum Post-Traumatic Stress Disorder is (PPTSD) associated with pregnancy. Approximately 9% of women experience postpartum post-traumatic stress disorder (PTSD) following childbirth.2
- Postpartum Traumatic Stress (PPTSD) Disorder
Approximately 9% of women experience postpartum post-traumatic stress disorder (PPTSD) following childbirth. Most often, this illness is caused by a real or perceived trauma during delivery or postpartum. These traumas could include:
- Prolapsed cord
- Unplanned C-section
- Use of vacuum extractor or forceps to deliver the baby
- Baby going to NICU
- Feelings of powerlessness, poor communication and/or lack of support and reassurance during the delivery
- Women who have experienced a previous trauma, such as rape or sexual abuse, are also at a higher risk for experiencing postpartum Traumatic Stress Disorder (PPTSD).
- Women who have experienced a severe physical complication or injury related to pregnancy or childbirth, such as severe postpartum hemorrhage, unexpected hysterectomy, severe preeclampsia/eclampsia, perineal trauma (3rd or 4th degree tear), or cardiac disease.
Symptoms of Postpartum Traumatic Stress Disorder (PPTSD) Symptoms of postpartum PTSD might include:
- Intrusive re-experiencing (re-living) of a past traumatic event (which in this case may have been the childbirth itself)
- Flashbacks or nightmares
- Avoidance of stimuli associated with the event, including thoughts, feelings, people, places and details of the event
- Persistent increased arousal (irritability, difficulty sleeping, hypervigilance, exaggerated startle response)
- Anxiety and panic attacks
- Feeling a sense of unreality and detachment
Postpartum PPTSD is distressful but treatable with professional help. If you feel you may be suffering from this illness, know that it is not your fault and you are not to blame.
- Postpartum Bipolar Disorder (Peripartum 'around the time of birth' Bipolar Disorder) is characterized by high and elevated mood episodes mania, hypomania or depression that can begin during pregnancy or in the weeks after childbirth. Early recognition of women with bipolar disorder in pregnancy is critical as the risk of postpartum depression is high. Working with a mental health clinician to use evidence-based therapy, appropriate medication, and bright light therapy is needed to treat bipolar disorder.
- Menopause and Mental Health:
Menopause is when your period stops permanently. Menopause is a normal part of a woman’s life. It is sometimes called “the change of life." Menopause does not happen all at once. As your body transitions to menopause over several years, you may have menopause symptoms and irregular periods. The average age for menopause in the United States is 52.
What is menopause?
Menopause is when your periods stop permanently and you can no longer get pregnant. You have reached menopause only after it has been a full year since your last period. This means you have not had any bleeding, including spotting, for 12 months in a row.
After menopause your ovaries make very low levels of the hormones estrogen and progesterone. These low hormone levels can raise your risk for certain health problems.
What is perimenopause, or the transition to menopause?
Perimenopause (PER-ee-MEN-oh-pawz), or the menopausal transition, is the time leading up to your last period. Perimenopause means “around menopause.”
Perimenopause is a long transition to menopause, or the time when your periods stop permanently and you can no longer get pregnant. As your body transitions to menopause, your hormone levels may change randomly, causing menopause symptoms unexpectedly. During this transition, your ovaries make different amounts of the hormones estrogen (ES-truh-jin) and progesterone (proh-JES-tuh-RONE) than usual.
Irregular periods happen during this time because you may not ovulate every month. Your periods may be longer or shorter than usual. You might skip a few months or have unusually long or short menstrual cycles. Your period may be heavier or lighter than before. Many women also have hot flashes and other menopause symptoms during this transition.
When does the transition to menopause usually start?
Perimenopause, the transition to menopause, usually starts in a woman's mid- to late 40s.1 On average, women are in perimenopause for four years before their periods stop.
How will I know if I am starting the transition to menopause?
Sometimes it can be hard for you and your doctor to tell whether you are in perimenopause, the transition to menopause:
Menopausal Symptoms: Tell your doctor or nurse about any menopause symptoms, such as hot flashes or trouble sleeping. Menopausal symptoms also include:
- Irregular periods: Track your periods. Irregular periods may be your first sign of menopause.
- Hormone levels: Your doctor may test the amount of hormones in your blood if your periods stopped at an early age (before 40). Doctors don’t usually recommend this test unless there is a medical reason to do so. This is because, for most women, hormone levels go up and down in an unpredictable way during the transition to menopause. So it is difficult to tell for sure whether you have gone through menopause or are getting close to it based on this blood test.
How will menopause affect me? Symptoms of menopause may begin suddenly and be very noticeable, or they may be very mild at first. Symptoms may happen most of the time once they begin, or they may happen only once in a while. Some women notice changes in many areas. Some menopausal symptoms, such as moodiness, are similar to symptoms of premenstrual syndrome (PMS). Others may be new to you. For example:
- Your menstrual periods may not come as regularly as before. They also might last longer or be shorter. You might skip some months. Periods might stop for a few months and then start up again.
- Your periods might be heavier or lighter than before.
- You might have hot flashes and problems sleeping.
- You might experience mood swings or be irritable.
- You might experience vaginal dryness. Sex may be uncomfortable or painful.
- You may have less interest in sex. It may take longer for you to get aroused.
Other possible changes are not as noticeable. For example, you might begin to lose bone density because you have less estrogen. This can lead to osteoporosis, a condition that causes bones to become weak and break easily. Changing estrogen levels can also raise cholesterol levels and increase your risk for heart disease and stroke.
Talk to your doctor about possible treatment for your menopause symptoms if they bother you.
How long does the transition to menopause last?
Perimenopause, the transition to menopause, can last between two and eight years before your periods stop permanently. For most women, this transition to menopause lasts about four years. You will know you have reached menopause only after it has been a full year since your last period. This means you have not had any bleeding, including spotting, for 12 months in a row.
Should I continue using birth control during the transition to menopause?
Yes. You can still get pregnant during perimenopause, the transition to menopause, even if you miss your period for a month or a few months. During perimenopause you may still ovulate, or release an egg, on some months.
But it is impossible to know for sure when you will ovulate. If you don’t want to get pregnant, you should continue to use birth control until one full year after your last period. Talk to your doctor about your birth control needs. Learn more about different birth control methods.
You can’t get pregnant after menopause, but anyone who has sex can get sexually transmitted infections (STIs, or STDs). If you are not in a monogamous relationship in which you and your partner have sex with each other and no one else, protect yourself by using a male condom or dental dam correctly every time you have vaginal, oral, or anal sex. After menopause you may be more likely to get an STI from sex without a condom. Vaginal dryness or irritation is more common after menopause and can cause small cuts or tears during sex, exposing you to STIs.
When does menopause usually happen?
Menopause happens when you have gone 12 months in a row without a period. The average age of menopause in the United States is 52. The range for women is usually between 45 and 58. One way to tell when you might go through menopause is the age your mother went through it.
Menopause may happen earlier if you never had children. Pregnancy, especially more than one pregnancy, may delay menopause. Menopause may also happen earlier if you Smoke. Studies show smoking can cause you to start menopause up to two years earlier than women who don’t smoke.
Certain health problems can also cause you to start menopause earlier.
Menopause usually happens on its own. However, you may enter menopause earlier than you normally would if you have had chemotherapy or surgery to remove both ovaries.
What happens after menopause?
After menopause you will no longer be able to get pregnant and you will no longer get a period. If you have any type of vaginal bleeding after menopause, you should see a doctor as soon as possible. Vaginal bleeding after menopause is not normal and can mean that you have a serious health problem.
You may experience any of the following after menopause:
- Low hormone levels. With menopause, your ovaries make very little of the hormones estrogen and progesterone. Because of changing hormone levels, you may develop certain health risks, including osteoporosis, heart disease, and stroke.
- Menopause symptoms instead of period problems. After menopause, most women get relief from period problems or menopause symptoms. However, you may still experience symptoms such as hot flashes because of changing estrogen levels. One recent study found that hot flashes can continue for up to 14 years after menopause.
- Vaginal dryness. Vaginal dryness may be more common post-menopause. Learn more about treatments for vaginal dryness.
When to call Sunshine Behavioral Medicine:
As much majority of women transition from women and maternal mental distress uneventfully, for a lot of reason, some do not recover well. For this group, the woman and maternal related mental distress is too high to overcome without medical and professional care. It is imperative for this group to seek medical help as soon as they or their significant relations notice that their mental distress is adversely affecting their personal care, their relations, their home, school and their work responsibility’s. In these situations, trying to go it alone will not help and mind over the matter has a limit. That is when to call Sunshine Behavioral Medicine where help is only moments away. Call 850-360-4147.
Avoid suffering in silence from the fear and worries of what others may think about seeking mental health services.
Contact us to schedule your assessment.